Pseudomembranous enterocolitis: Difference between revisions
imported>Robert Badgett |
imported>Robert Badgett |
||
| Line 16: | Line 16: | ||
==Treatment== | ==Treatment== | ||
===Antibiotics=== | ===Antibiotics=== | ||
Various antibiotics have been studied.<ref name="pmid17636768">{{cite journal |author=Nelson R |title=Antibiotic treatment for Clostridium difficile-associated diarrhea in adults |journal=Cochrane Database Syst Rev |volume= |issue=3 |pages=CD004610 |year=2007 |pmid=17636768 |doi=10.1002/14651858.CD004610.pub3 |url=http://dx.doi.org/10.1002/14651858.CD004610.pub3 |issn=}}</ref><ref name="pmid8722937">{{cite journal |author=Wenisch C, Parschalk B, Hasenhündl M, Hirschl AM, Graninger W |title=Comparison of vancomycin, teicoplanin, metronidazole, and fusidic acid for the treatment of Clostridium difficile-associated diarrhea |journal=Clin. Infect. Dis. |volume=22 |issue=5 |pages=813–8 |year=1996 |month=May |pmid=8722937 |doi= |url= |issn=}}</ref><ref name=" | Various antibiotics have been studied in [[randomized controlled trial]]s.<ref name="pmid17636768">{{cite journal |author=Nelson R |title=Antibiotic treatment for Clostridium difficile-associated diarrhea in adults |journal=Cochrane Database Syst Rev |volume= |issue=3 |pages=CD004610 |year=2007 |pmid=17636768 |doi=10.1002/14651858.CD004610.pub3 |url=http://dx.doi.org/10.1002/14651858.CD004610.pub3 |issn=}}</ref><ref name="pmid8722937">{{cite journal |author=Wenisch C, Parschalk B, Hasenhündl M, Hirschl AM, Graninger W |title=Comparison of vancomycin, teicoplanin, metronidazole, and fusidic acid for the treatment of Clostridium difficile-associated diarrhea |journal=Clin. Infect. Dis. |volume=22 |issue=5 |pages=813–8 |year=1996 |month=May |pmid=8722937 |doi= |url= |issn=}}</ref><ref name="pmid19133801">{{cite journal |author=Musher DM, Logan N, Bressler AM, Johnson DP, Rossignol JF |title=Nitazoxanide versus Vancomycin in Clostridium difficile Infection: A Randomized, Double-Blind Study |journal=Clin. Infect. Dis. |volume= |issue= |pages= |year=2009 |month=January |pmid=19133801 |doi=10.1086/596552 |url=http://www.journals.uchicago.edu/doi/abs/10.1086/596552?url_ver=Z39.88-2003&rfr_id=ori:rid:crossref.org&rfr_dat=cr_pub%3dncbi.nlm.nih.gov |issn=}}</ref> [[Teicoplanin]] may be the most effective antibiotic.<ref name="pmid17636768">{{cite journal |author=Nelson R |title=Antibiotic treatment for Clostridium difficile-associated diarrhea in adults |journal=Cochrane Database Syst Rev |volume= |issue=3 |pages=CD004610 |year=2007 |pmid=17636768 |doi=10.1002/14651858.CD004610.pub3 |url=http://dx.doi.org/10.1002/14651858.CD004610.pub3 |issn=}}</ref><ref name="pmid8722937">{{cite journal |author=Wenisch C, Parschalk B, Hasenhündl M, Hirschl AM, Graninger W |title=Comparison of vancomycin, teicoplanin, metronidazole, and fusidic acid for the treatment of Clostridium difficile-associated diarrhea |journal=Clin. Infect. Dis. |volume=22 |issue=5 |pages=813–8 |year=1996 |month=May |pmid=8722937 |doi= |url= |issn=}}</ref> [[Vancomycin]] has an insignificant trend towards being better than [[metronidazole]].<ref name="pmid17636768">{{cite journal |author=Nelson R |title=Antibiotic treatment for Clostridium difficile-associated diarrhea in adults |journal=Cochrane Database Syst Rev |volume= |issue=3 |pages=CD004610 |year=2007 |pmid=17636768 |doi=10.1002/14651858.CD004610.pub3 |url=http://dx.doi.org/10.1002/14651858.CD004610.pub3 |issn=}}</ref> | ||
===Administration of bacteria=== | ===Administration of bacteria=== | ||
[[ | [[Probiotic]] administration may<ref name="pmid16635227">{{cite journal |author=McFarland LV |title=Meta-analysis of probiotics for the prevention of antibiotic associated diarrhea and the treatment of Clostridium difficile disease |journal=Am. J. Gastroenterol. |volume=101 |issue=4 |pages=812–22 |year=2006 |month=April |pmid=16635227 |doi=10.1111/j.1572-0241.2006.00465.x |url=http://dx.doi.org/10.1111/j.1572-0241.2006.00465.x |issn=}}</ref> or may not <ref name="pmid18254055">{{cite journal |author=Pillai A, Nelson R |title=Probiotics for treatment of Clostridium difficile-associated colitis in adults |journal=Cochrane Database Syst Rev |volume= |issue=1 |pages=CD004611 |year=2008 |pmid=18254055 |doi=10.1002/14651858.CD004611.pub2 |url=http://dx.doi.org/10.1002/14651858.CD004611.pub2 |issn=}}</ref>help according to a [[meta-analysis|meta-analyses]] and a more recent [[randomized controlled trial]].<ref name="pmid18840110">{{cite journal |author=Klarin B, Wullt M, Palmquist I, Molin G, Larsson A, Jeppsson B |title=Lactobacillus plantarum 299v reduces colonisation of Clostridium difficile in critically ill patients treated with antibiotics |journal=Acta Anaesthesiol Scand |volume=52 |issue=8 |pages=1096–102 |year=2008 |month=September |pmid=18840110 |doi=10.1111/j.1399-6576.2008.01748.x |url=http://dx.doi.org/10.1111/j.1399-6576.2008.01748.x |issn=}}</ref> | ||
Rectal infusion of feces helped | ===Recurrent infection=== | ||
A [[clinical prediction rule]] found that recurrent infection is more likely if age is more than 65 years, the patient has severe or fulminant illness, and additional antibiotic exposure occurs after after treatment of the initial Clostridium difficile infection.<ref name="pmid19162027">{{cite journal |author=Hu MY, Katchar K, Kyne L, ''et al'' |title=Prospective Derivation and Validation of a Clinical Prediction Rule for Recurrent Clostridium difficile Infection |journal=Gastroenterology |volume= |issue= |pages= |year=2008 |month=December |pmid=19162027 |doi=10.1053/j.gastro.2008.12.038 |url=http://linkinghub.elsevier.com/retrieve/pii/S0016-5085(08)02262-2 |issn=}}</ref> Use of antacids may also be a risk factor for recurrence.<ref name="pmid18951661">{{cite journal |author=Garey KW, Sethi S, Yadav Y, DuPont HL |title=Meta-analysis to assess risk factors for recurrent Clostridium difficile infection |journal=J. Hosp. Infect. |volume=70 |issue=4 |pages=298–304 |year=2008 |month=December |pmid=18951661 |doi=10.1016/j.jhin.2008.08.012 |url=http://linkinghub.elsevier.com/retrieve/pii/S0195-6701(08)00352-6 |issn=}}</ref> | |||
Observational studies conflict regarding the best agent and suggest [[vancomycin]] may<ref name="pmid12135033">{{cite journal |author=McFarland LV, Elmer GW, Surawicz CM |title=Breaking the cycle: treatment strategies for 163 cases of recurrent Clostridium difficile disease |journal=Am. J. Gastroenterol. |volume=97 |issue=7 |pages=1769–75 |year=2002 |month=July |pmid=12135033 |doi=10.1016/S0002-9270(02)04195-3 |url= |issn=}}</ref> or may not<ref name="pmid16477549">{{cite journal |author=Pépin J, Routhier S, Gagnon S, Brazeau I |title=Management and outcomes of a first recurrence of Clostridium difficile-associated disease in Quebec, Canada |journal=Clin. Infect. Dis. |volume=42 |issue=6 |pages=758–64 |year=2006 |month=March |pmid=16477549 |doi=10.1086/501126 |url=http://www.journals.uchicago.edu/doi/abs/10.1086/501126?url_ver=Z39.88-2003&rfr_id=ori:rid:crossref.org&rfr_dat=cr_pub%3dncbi.nlm.nih.gov |issn=}}</ref> be better than [[metronidazole]]. Various methods exist for the administration of [[vancomycin]]<ref name="pmid12135033">{{cite journal |author=McFarland LV, Elmer GW, Surawicz CM |title=Breaking the cycle: treatment strategies for 163 cases of recurrent Clostridium difficile disease |journal=Am. J. Gastroenterol. |volume=97 |issue=7 |pages=1769–75 |year=2002 |month=July |pmid=12135033 |doi=10.1016/S0002-9270(02)04195-3 |url= |issn=}}</ref> | |||
Serial therapy with [[vancomycin]] and [[rifaximin]] has been studied in a small uncontrolled series of patients.<ref name="pmid17304459">{{cite journal |author=Johnson S, Schriever C, Galang M, Kelly CP, Gerding DN |title=Interruption of recurrent Clostridium difficile-associated diarrhea episodes by serial therapy with vancomycin and rifaximin |journal=Clin. Infect. Dis. |volume=44 |issue=6 |pages=846–8 |year=2007 |month=March |pmid=17304459 |doi=10.1086/511870 |url=http://www.journals.uchicago.edu/doi/abs/10.1086/511870?url_ver=Z39.88-2003&rfr_id=ori:rid:crossref.org&rfr_dat=cr_pub%3dncbi.nlm.nih.gov |issn=}}</ref> | |||
====Administration of bacteria==== | |||
Rectal infusion of feces helped according to case reports.<ref name="pmid6137662">{{cite journal |author=Schwan A, Sjölin S, Trottestam U, Aronsson B |title=Relapsing clostridium difficile enterocolitis cured by rectal infusion of homologous faeces |journal=Lancet |volume=2 |issue=8354 |pages=845 |year=1983 |month=October |pmid=6137662 |doi= |url=http://linkinghub.elsevier.com/retrieve/pii/S0140-6736(83)90753-5 |issn=}}</ref><ref name="pmid18808083">{{cite journal |author=Nieuwdorp M, van Nood E, Speelman P, ''et al'' |title=[Treatment of recurrent Clostridium difficile-associated diarrhoea with a suspension of donor faeces] |language=Dutch; Flemish |journal=Ned Tijdschr Geneeskd |volume=152 |issue=35 |pages=1927–32 |year=2008 |month=August |pmid=18808083 |doi= |url= |issn=}}</ref> | |||
==References== | ==References== | ||
<references/> | <references/> | ||
Revision as of 10:47, 2 February 2009
| Pseudomembranous enterocolitis | |
|---|---|
| Pseudomembranous enterocolitis | |
| MeSH | D004761 |
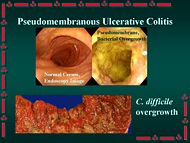
In medicine, pseudomembranous enterocolitis is an "acute inflammation of the intestinal mucosa that is characterized by the presence of pseudomembranes or plaques in the small intestine (pseudomembranous enteritis) and the large intestine (pseudomembranous colitis). It is commonly associated with antibiotic therapy and clostridium difficile colonization."[1]
Treatment
Antibiotics
Various antibiotics have been studied in randomized controlled trials.[2][3][4] Teicoplanin may be the most effective antibiotic.[2][3] Vancomycin has an insignificant trend towards being better than metronidazole.[2]
Administration of bacteria
Probiotic administration may[5] or may not [6]help according to a meta-analyses and a more recent randomized controlled trial.[7]
Recurrent infection
A clinical prediction rule found that recurrent infection is more likely if age is more than 65 years, the patient has severe or fulminant illness, and additional antibiotic exposure occurs after after treatment of the initial Clostridium difficile infection.[8] Use of antacids may also be a risk factor for recurrence.[9]
Observational studies conflict regarding the best agent and suggest vancomycin may[10] or may not[11] be better than metronidazole. Various methods exist for the administration of vancomycin[10]
Serial therapy with vancomycin and rifaximin has been studied in a small uncontrolled series of patients.[12]
Administration of bacteria
Rectal infusion of feces helped according to case reports.[13][14]
References
- ↑ Anonymous (2024), Pseudomembranous enterocolitis (English). Medical Subject Headings. U.S. National Library of Medicine.
- ↑ 2.0 2.1 2.2 Nelson R (2007). "Antibiotic treatment for Clostridium difficile-associated diarrhea in adults". Cochrane Database Syst Rev (3): CD004610. DOI:10.1002/14651858.CD004610.pub3. PMID 17636768. Research Blogging.
- ↑ 3.0 3.1 Wenisch C, Parschalk B, Hasenhündl M, Hirschl AM, Graninger W (May 1996). "Comparison of vancomycin, teicoplanin, metronidazole, and fusidic acid for the treatment of Clostridium difficile-associated diarrhea". Clin. Infect. Dis. 22 (5): 813–8. PMID 8722937. [e]
- ↑ Musher DM, Logan N, Bressler AM, Johnson DP, Rossignol JF (January 2009). "Nitazoxanide versus Vancomycin in Clostridium difficile Infection: A Randomized, Double-Blind Study". Clin. Infect. Dis.. DOI:10.1086/596552. PMID 19133801. Research Blogging.
- ↑ McFarland LV (April 2006). "Meta-analysis of probiotics for the prevention of antibiotic associated diarrhea and the treatment of Clostridium difficile disease". Am. J. Gastroenterol. 101 (4): 812–22. DOI:10.1111/j.1572-0241.2006.00465.x. PMID 16635227. Research Blogging.
- ↑ Pillai A, Nelson R (2008). "Probiotics for treatment of Clostridium difficile-associated colitis in adults". Cochrane Database Syst Rev (1): CD004611. DOI:10.1002/14651858.CD004611.pub2. PMID 18254055. Research Blogging.
- ↑ Klarin B, Wullt M, Palmquist I, Molin G, Larsson A, Jeppsson B (September 2008). "Lactobacillus plantarum 299v reduces colonisation of Clostridium difficile in critically ill patients treated with antibiotics". Acta Anaesthesiol Scand 52 (8): 1096–102. DOI:10.1111/j.1399-6576.2008.01748.x. PMID 18840110. Research Blogging.
- ↑ Hu MY, Katchar K, Kyne L, et al (December 2008). "Prospective Derivation and Validation of a Clinical Prediction Rule for Recurrent Clostridium difficile Infection". Gastroenterology. DOI:10.1053/j.gastro.2008.12.038. PMID 19162027. Research Blogging.
- ↑ Garey KW, Sethi S, Yadav Y, DuPont HL (December 2008). "Meta-analysis to assess risk factors for recurrent Clostridium difficile infection". J. Hosp. Infect. 70 (4): 298–304. DOI:10.1016/j.jhin.2008.08.012. PMID 18951661. Research Blogging.
- ↑ 10.0 10.1 McFarland LV, Elmer GW, Surawicz CM (July 2002). "Breaking the cycle: treatment strategies for 163 cases of recurrent Clostridium difficile disease". Am. J. Gastroenterol. 97 (7): 1769–75. DOI:10.1016/S0002-9270(02)04195-3. PMID 12135033. Research Blogging.
- ↑ Pépin J, Routhier S, Gagnon S, Brazeau I (March 2006). "Management and outcomes of a first recurrence of Clostridium difficile-associated disease in Quebec, Canada". Clin. Infect. Dis. 42 (6): 758–64. DOI:10.1086/501126. PMID 16477549. Research Blogging.
- ↑ Johnson S, Schriever C, Galang M, Kelly CP, Gerding DN (March 2007). "Interruption of recurrent Clostridium difficile-associated diarrhea episodes by serial therapy with vancomycin and rifaximin". Clin. Infect. Dis. 44 (6): 846–8. DOI:10.1086/511870. PMID 17304459. Research Blogging.
- ↑ Schwan A, Sjölin S, Trottestam U, Aronsson B (October 1983). "Relapsing clostridium difficile enterocolitis cured by rectal infusion of homologous faeces". Lancet 2 (8354): 845. PMID 6137662. [e]
- ↑ Nieuwdorp M, van Nood E, Speelman P, et al (August 2008). "[Treatment of recurrent Clostridium difficile-associated diarrhoea with a suspension of donor faeces]" (in Dutch; Flemish). Ned Tijdschr Geneeskd 152 (35): 1927–32. PMID 18808083. [e]